Obesity is a disease that can be driven by factors beyond an individual’s control3
Some factors include3,4:

Epigenetic

Sociocultural

Environmental

Physiological

Behavioral

Genetic
Lifestyle modification alone may not be enough to treat adults with obesity5
The body may resist weight loss5
- When patients restrict calories to reduce weight, the body may compensate for that calorie restriction by altering appetite-regulating hormones and the desire to eat5
Are your employees getting the care they need?
Recent studies have found that workplace well-being programs did not address many clinical health measures6,7
Employees in 2 studies across 2 industries showed changes in self-reported health behaviors with workplace well-being programs, including engaging in regular exercise, managing their weight, and having a primary care physician.6,7 However, the programs did not lead to detectable effects on measures including:
Additionally, there were no detectable effects on waist circumference,7 lipids,6,7 or blood pressure.6,7
Zepbound is not indicated for dyslipidemia or hypertension.
The first of the 2 studies was a randomized trial of a multiyear, multicomponent workplace well-being program utilized by employees of a large US warehouse retail company between January 2015 and June 2016 (N=32,974). Twenty treatment sites were randomly selected, with the remaining sites acting as the control with no well-being program. The well-being program, designed and implemented by the well-being vendor Wellness Workdays, comprised 8 modules lasting 4 to 8 weeks each, implemented over 18 months by registered dietitians through individual and team-based activities, with modest incentives for participation.6 The second study was a randomized controlled trial of a workplace well-being program for employees at the University of Illinois at Urbana-Champaign from August 2016 to April 2018 (N=4834). Employees were randomly assigned to the treatment or control groups. The treatment group was eligible to participate in a comprehensive workplace well-being program, iThrive, which was designed to be representative of typical programs offered by employers with 3 annual components: an on-site biometric screening and survey, an online health risk assessment, and a choice of well-being activities.7
Consider how anti-obesity medications (AOMs) could help the employees in your organization. Give your employees access to AOMs.
Anti-obesity medications act as a complement to–not a substitute for–a reduced-calorie diet and increased physical activity2,8
Professional society recommendations for the management of obesity regarding pharmacological intervention

More recent guidelines from 2022 by the ASMBS and IFSO recommend bariatric surgery for patients with a BMI of ≥35 kg/m2 with or without comorbidities and recommend considering bariatric surgery for patients with a BMI of 30 to 34.9 kg/m2 and metabolic disease.9
Table depicting AACE/ACE and Endocrine Society recommendations for lifestyle interventions (adjustments to diet, exercise, and behavior are the basis for treatment), anti-obesity medications (adjunct to lifestyle modification as part of a comprehensive management strategy), and bariatric surgery (adjunct to lifestyle modification and AOMs as part of a comprehensive management strategy). AACE/ACE recommends lifestyle interventions for BMI ≥25 kg/m2, AOMs for BMI ≥27 kg/m2 with comorbidities or for BMI ≥30 kg/m2 with or without comorbidities, and bariatric surgery for BMI ≥35 kg/m2 with ≥1 severe obesity-related complication. Endocrine Society recommends lifestyle interventions for BMI ≥25 kg/m2, AOMs for BMI ≥27 kg/m2 with comorbidity or for BMI ≥30 kg/m2 with or without comorbidity, and bariatric surgery for BMI ≥35 kg/m2 with comorbidity or BMI ≥40 kg/m2.
a2016 AACE/ACE guidelines for obesity recommend bariatric surgery for patients with a BMI of ≥40 kg/m2 without coexisting medical problems and for whom the procedure would not be associated with excessive risk, and they recommend considering a bariatric procedure for patients with a BMI of ≥35 kg/m2 and 1 or more severe obesity-related complications. The guidelines also recommend considering a bariatric procedure for patients with a BMI of 30 kg/m2 to 34.9 kg/m2 who have diabetes or metabolic syndrome, but note that current evidence is limited by the number of patients studied and a lack of long-term data demonstrating net benefit.2
AACE=American Association of Clinical Endocrinology; ACE=American College of Endocrinology; AOMs=anti-obesity medication; ASMBS=American Society of Metabolic and Bariatric Surgery; BMI=body mass index; IFSO=International Federation for the Surgery of Obesity and Metabolic Disorders.
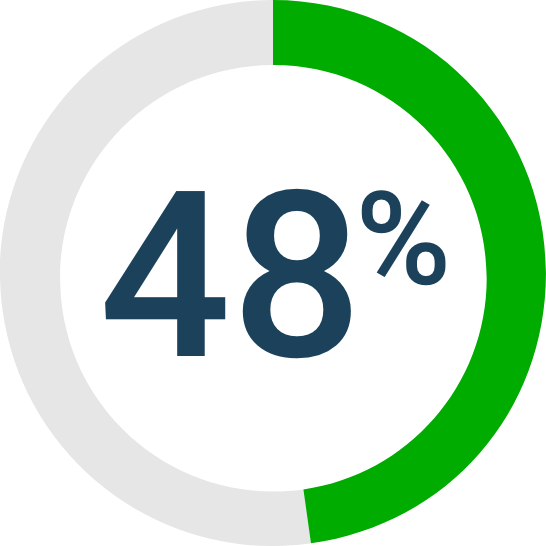
48% of large employers are covering branded anti-obesity medications10*
*Based on a 2023 survey of 109 employers with 5000 to 100,000+ US employees and 5.4 million covered lives.10
Respondents were asked if their organization provided insurance coverage for branded weight loss medications.10
References
-
Centers for Disease Control and Prevention. About overweight & obesity. Updated February 24, 2023. Accessed
July 7, 2023.
https://www.cdc.gov
/obesity /about-obesity /index.html - Garvey WT, Mechanick JI, Brett EM, et al. American Association of Clinical Endocrinologists and American College of Endocrinology comprehensive clinical practice guidelines for medical care of patients with obesity. Endocr Pract. 2016;22(suppl 3):1-203.
-
Centers for Disease Control and Prevention. Causes of obesity. Updated March 21, 2022. Accessed June 17,
2023.
https://www.cdc.gov
/obesity /basics /causes.html - Mahmoud AM. An overview of epigenetics in obesity: the role of lifestyle and therapeutic interventions. Int J Mol Sci. 2022;23(3):1341.
- Apovian CM, Aronne LJ, Bessesen DH, et al. Pharmacological management of obesity: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2015;100(2):342-362.
- Song ZS, Baicker K. Effect of a workplace wellness program on employee health and economic outcomes: a randomized clinical trial. JAMA. 2019;321(15):1491-1501.
- Reif J, Chan D, Jones D, Payne L, Molitor D. Effects of a workplace wellness program on employee health, health beliefs, and medical use: a randomized clinical trial. JAMA Intern Med. 2020;180(7):952-960
- Perdomo CM, Cohen RV, Sumithran P, Clément K, Frühbeck G. Contemporary medical, device, and surgical therapies for obesity in adults. Lancet. 2023;401(10382):1116-1130
- Eisenberg D, Shikora SA, Aarts E, et al. 2022 American Society for Metabolic and Bariatric Surgery (ASMBS) and International Federation for the Surgery of Obesity and Metabolic Disorders (IFSO): indications for metabolic and bariatric surgery. Surg Obes Relat Dis. 2022;18(12):1345-1356.
- Data on file. Lilly USA, LLC. DOF-ZP-US-0011.




